Meet Mr Bipin. He is nearing 62. These days, he pauses before signing his name, his hand trembling as he tries to steady the pen. What was once a simple task now takes great effort. His movements have slowed, his steps have become shorter, and at times he shuffles or loses balance without warning.Mr Bipin, who once never missed his evening walk around the house, now skips it almost every day. His body often feels stiff, his face less expressive than before. At night, his sleep is restless, and during the day, an unshakeable fatigue and anxiety leave him constantly unsettled and drained.At first, the signs are easy to dismiss as aging, stress, or just “weakness,” as some say. The sudden tremor draws curious glances, the slowness draws impatience, even from his family members at times. Conversations begin to feel effortful, and gradually, he starts withdrawing, reluctant to explain what he himself doesn’t fully understand.For months, the symptoms remain unnamed, often dismissed as stress or ageing, until a clinical diagnosis brings difficult clarity: he has Parkinson’s disease, one of the fastest-growing neurological conditions globally, affecting nearly 10 million people worldwide.
What is Parkinson’s disease?
According to WHO, Parkinson’s disease (PD) is a progressive neurodegenerative brain disorder that causes problems with movement, mental health, sleep, pain and other health issues.It develops when nerve cells in a part of the brain called the substantia nigra gradually become damaged or die. These cells normally produce dopamine, a chemical that helps coordinate smooth and controlled muscle movement. As dopamine levels decrease, the brain’s ability to regulate movement becomes impaired.The condition most commonly affects motor skills, coordination, and causes tremors (involuntary shaking), slowness of movement (bradykinesia), muscle stiffness, and problems with balance and coordination. Over time, people may also experience changes in posture, reduced facial expression, softer speech, and smaller handwriting. Beyond movement-related symptoms, Parkinson’s can also affect sleep, cognition, hearing ability, mood, memory, and overall energy levels.Parkinson’s disease is long-term and progressive, meaning symptoms typically worsen gradually over time, though the rate of progression varies widely from person to person.
What causes Parkinson’s disease?
The exact cause of Parkinson’s disease is still not fully understood. It is now widely accepted that the condition develops due to a combination of biological changes in the brain, along with genetic and environmental risk factors over time.At the core of the disease is the gradual loss of dopamine-producing neurons in a region of the brain called the substantia nigra. This leads to reduced dopamine levels, which disrupt the brain circuits responsible for smooth and coordinated movement.Another key feature seen in Parkinson’s is the abnormal accumulation of a protein called alpha-synuclein. This protein forms clumps known as Lewy bodies inside nerve cells and is strongly linked to nerve cell dysfunction and degeneration.Researchers believe several factors may contribute to these changes, including age, genetic susceptibility in a small proportion of cases, and environmental exposures such as pesticides and certain toxins. However, no single cause has been identified, and in most patients, the disease appears to develop sporadically without a clear trigger.
Beyond tremors: The hidden side of Parkinson’s
Parkinson’s is often associated with visible symptoms: tremors, stiffness, and slowed movement. But medically, it is a progressive neurological condition that begins deep within the brain. It develops when nerve cells that produce dopamine, a chemical essential for smooth, coordinated movement, gradually deteriorate. As dopamine levels fall, the brain’s ability to control movement and coordination weakens.
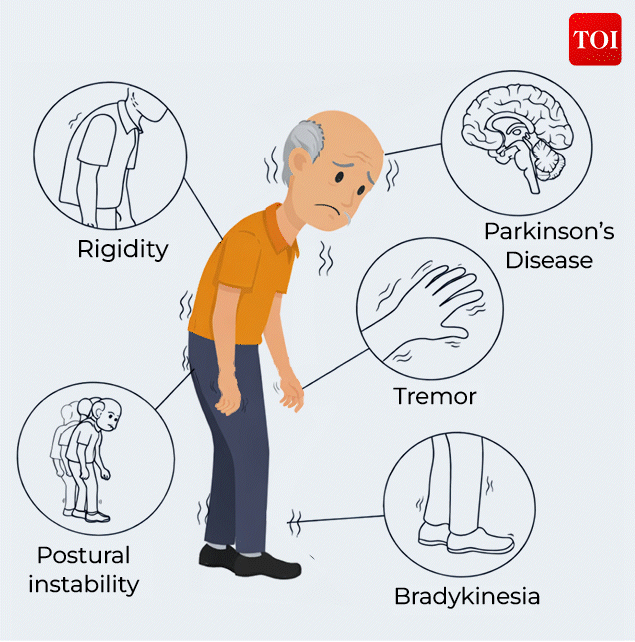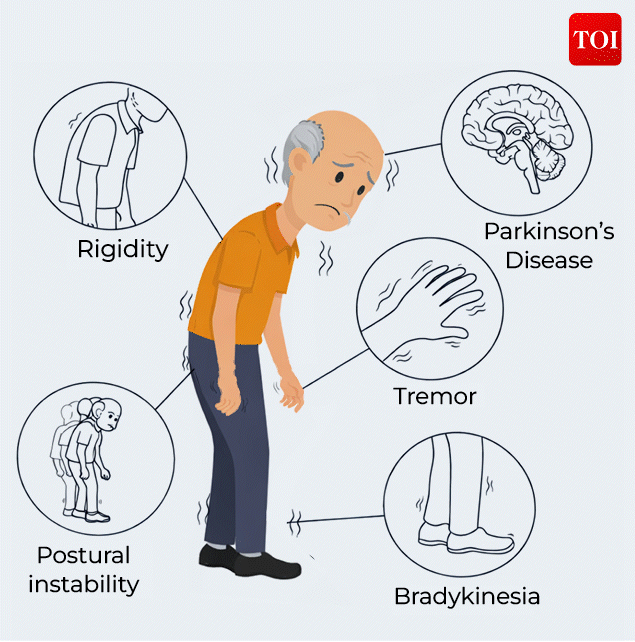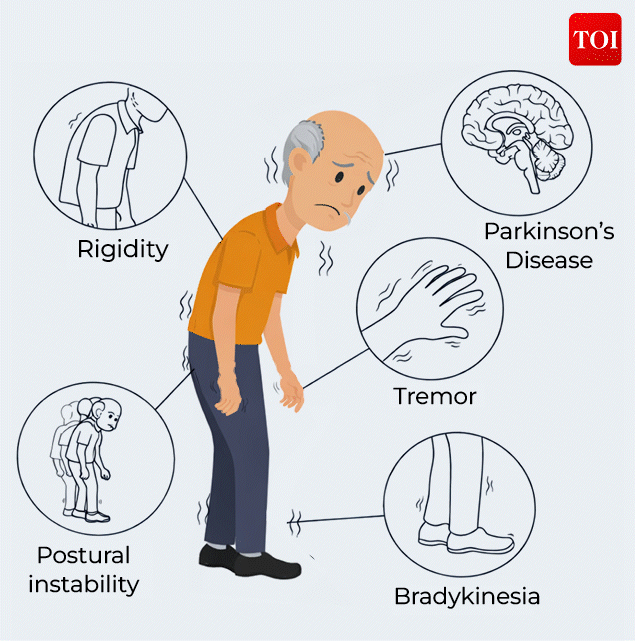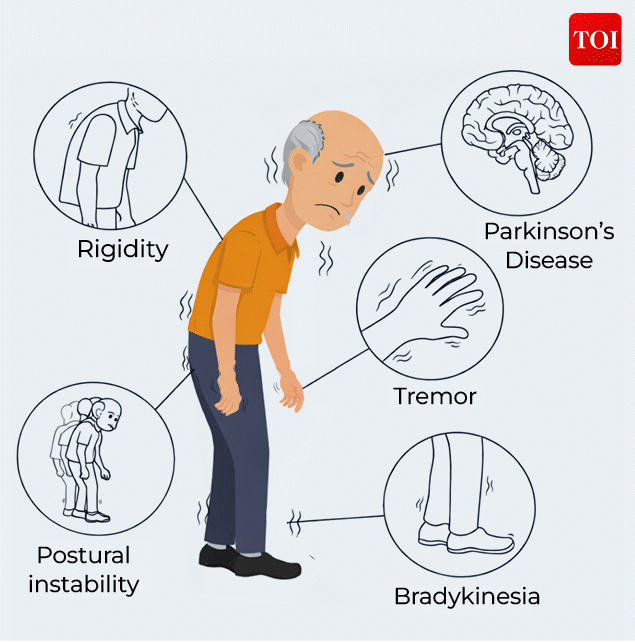
Parkinson’s disease
While motor symptoms are the most recognisable, the disease extends far beyond movement. Non-motor symptoms, often subtle and easy to miss, can appear years before tremors or stiffness. These include sleep disturbances, fatigue, mood changes, loss of smell, and cognitive slowing, making Parkinson’s as much a behavioural and psychological condition as a physical one.
Non-motor symptoms: the missed early warning signs
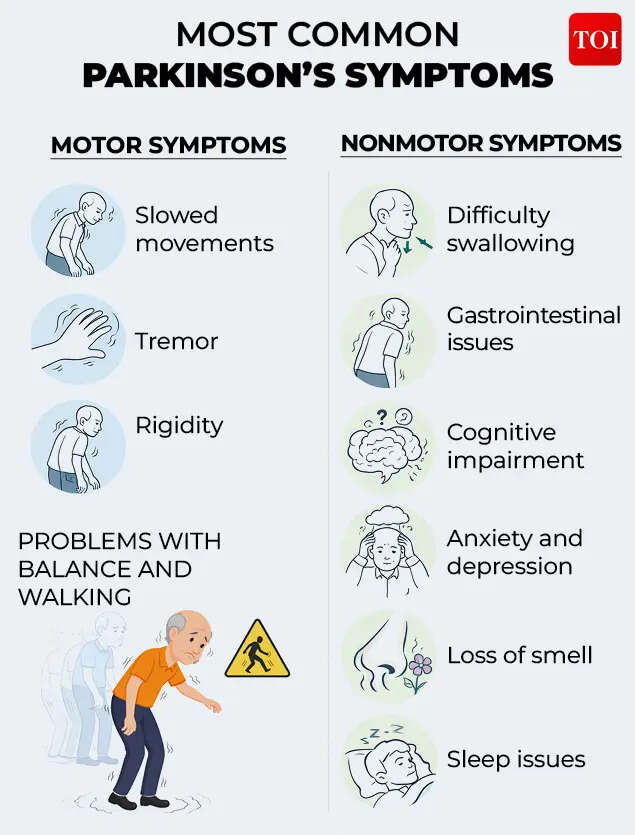
Speaking to TOI, Dr Riaz Ahamed Syed, paediatric neurologist with over four decades of experience, explained that Parkinson’s is often misunderstood as a movement disorder alone, while a large part of its burden comes from symptoms that are less visible.“Most people think of tremors, rigidity, and slowness. But a large part of the disease lies in non-motor symptoms, which are frequently missed,” he said.According to him, mood-related changes such as anxiety, depression, and apathy, along with slowing of thought and cognitive decline, are common but under-recognised. Patients may also experience loss of smell, constipation, urinary urgency, sleep disturbances, and difficulty swallowing, symptoms that can appear years before the classic motor signs.
.
“These symptoms are non-specific and often ignored. But if recognised early, we can begin treatment sooner and manage the condition better,” he added.
Treatment and managing symptoms
Parkinson’s is a progressive and degenerative condition, meaning symptoms tend to worsen over time. At present, there is no definitive cure, but treatment can significantly improve quality of life.“In younger patients, we may start with dopamine agonists, which help increase dopamine activity in the brain. After the age of 50, medications like levodopa are more commonly used,” Dr Syed explained.Other drugs, including MAO inhibitors and amantadine, may also be prescribed depending on the patient’s condition. In more advanced cases, therapies like deep brain stimulation can help control severe tremors.“The focus should be on consistent medication, regular follow-ups, and proper management, rather than looking for a permanent cure,” he said.
Who is at risk?
Age remains the strongest risk factor, with most cases developing after the age of 60. However, Parkinson’s is not exclusively a disease of the elderly; early-onset cases can occur, sometimes even before 50.The exact cause remains unclear, but experts believe a mix of genetic predisposition and environmental exposure plays a role. Individuals with a family history of Parkinson’s may have a higher risk, as may those exposed to certain toxins or pesticides over time.Men are slightly more likely to develop the condition than women, though the reasons are still being studied.Despite these risk factors, many patients, like Mr Bipin, develop Parkinson’s without any clear warning or identifiable cause.
The invisible burden: Caregiving and social stigma
Beyond the physical symptoms lies a deeper, often unspoken challenge: social and emotional isolation.Patients may gradually withdraw from social interactions, not because they want to, but because the disease makes communication and movement difficult. Slowed speech, reduced facial expressions, and physical limitations can be misinterpreted as disinterest or disengagement.“Patients tend to withdraw, and families sometimes don’t understand why,” Dr Syed said.Where awareness remains limited, this can lead to stigma, misunderstanding, and delayed care. At the same time, it can add to the emotional and physical toll on families taking on the role of caregivers, managing medications, daily routines, and emotional needs.
Everyday challenges
Parkinson’s affects even the simplest daily activities. Tasks like getting up from a chair, turning while walking, going to the washroom, or swallowing food can become difficult.“One misconception is that patients should try to move faster. This can actually increase the risk of falls,” Dr Syed cautioned.He emphasised the need to adapt the environment, from using assistive devices to modifying diets. Soft or semi-solid foods can help those with swallowing difficulties, while fibre-rich diets can ease constipation, a common issue.Physiotherapy and rehabilitation, he added, are essential in maintaining mobility and independence.
The “million-dollar question”: Can Parkinson’s disease be cured ?
Dr Syed addressed one of the most frequently asked concerns, which he referred to as the “million-dollar question” asked by patients and families about whether Parkinson’s disease has a permanent cure. He explained that it is a progressive, degenerative disorder that worsens over time and currently has no definitive cure, though treatment can help manage symptoms and improve quality of life.“The million-dollar question being asked is, Doc, can I have a permanent cure? We all know Parkinson’s disease is a progressive disorder, a degenerative disorder, and as years go by, patients tend to deteriorate. There are staging processes of Parkinson’s being done. But the million-dollar question is: can I have a permanent cure? Unfortunately, at this point in time, there is no specific cure for Parkinson’s disease.”While there is currently no cure, a combination of medications, physical therapy, lifestyle adjustments, and, in some cases, surgical treatments can help manage symptoms and improve quality of life.
Why this conversation matters now
On World Parkinson’s Day, the focus is not just on the disease itself, but on awareness, early detection, and support systems.According to a study titled Neuropalliative Care for Parkinson’s Disease in India, the prevalence of Parkinson’s disease (PD) in India accounts for roughly 10% of the global burden, making it a significant public health concern.Experts at the 6th International Annual Symposium-2026 in Kerala said that India is expected to witness a surge in Parkinson’s cases in the coming years, which may pose a growing burden on families and caregivers. Yet awareness of early symptoms and non-motor signs remains low.The need is not only for better treatment, but for earlier recognition, reduced stigma, and stronger support networks, so that patients are not left navigating the condition in silence.
Looking ahead
While there is no cure yet, ongoing research offers cautious optimism. New drug delivery systems and emerging therapies, including stem cell research particularly induced pluripotent stem cells and human pluripotent stem cells, are being explored.For now, doctors emphasise a holistic approach, combining medication, mental health support, physiotherapy, and family involvement.“Parkinson’s is not just about tremors or movement. It affects the entire life of the patient and the family,” Dr Syed said.Parkinson’s disease is increasingly being recognised as a condition that begins long before visible symptoms such as tremors appear. Evidence suggests that more than half of dopamine-producing neurons in the brain may already be lost by the time a clinical diagnosis is made, underlining how silently the disease progresses in its early stages.This makes early recognition of non-motor symptoms such as sleep disturbances, loss of smell, mood changes, and constipation especially important. Greater awareness among families and caregivers can help ensure earlier medical attention, timely diagnosis, and better symptom management.At the same time, experts emphasise that medical care alone is not enough. Social acceptance and understanding play a critical role, as patients often face isolation due to slowed speech, reduced facial expression, and movement difficulties that are frequently misunderstood. Reducing stigma can go a long way in improving mental well-being and quality of life.